
Denial Prevention & Resolution
Denial Prevention & Resolution focuses on strategies to minimize claim denials in healthcare revenue cycles and efficiently resolve those that occur. Effective programs combine proactive measures, data analysis, and staff training to boost reimbursements.
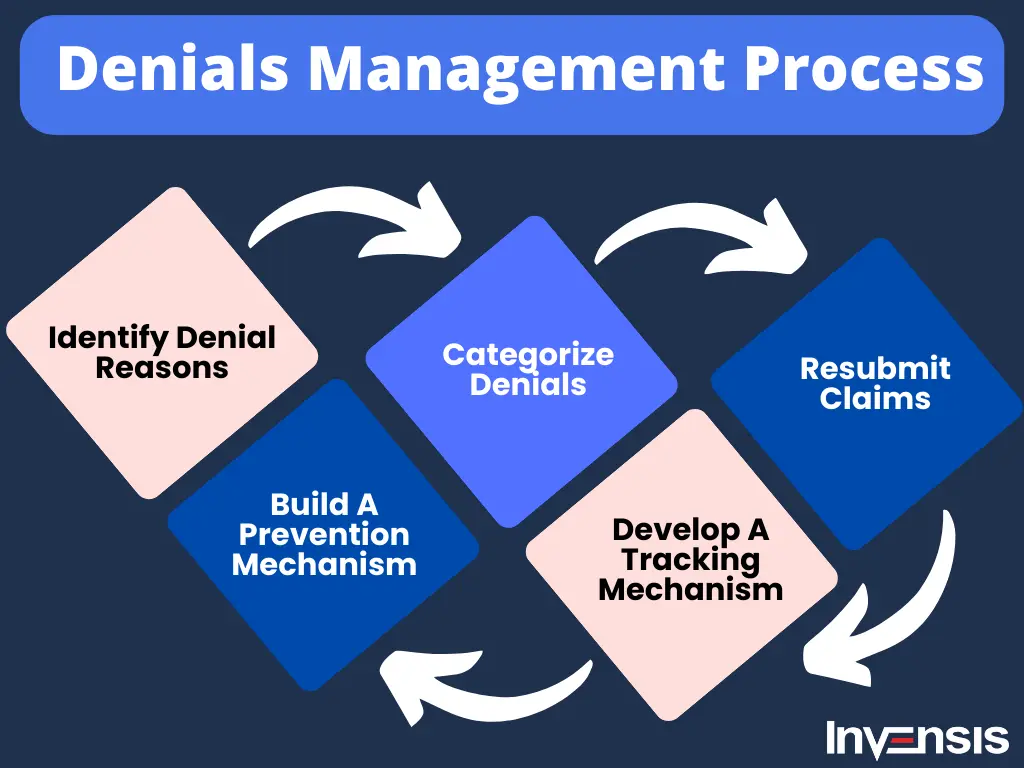
Proactive denial prevention starts with accurate data entry, insurance verification, and adherence to payer guidelines from the outset. Implement claim scrubbing tools to catch errors like coding mismatches before submission, reducing denials by up to 50% in many practices. Regular staff training on coding updates and documentation ensures compliance and minimizes front-end errors.
Denial Prevention & Resolution is a specialized Revenue Cycle Management (RCM) service focused on reducing claim denials and recovering lost revenue. It ensures that medical claims are submitted correctly the first time and that denied claims are quickly analyzed, corrected, and resubmitted for reimbursement. Healthcare organizations often lose revenue due to coding errors, incomplete documentation, eligibility issues, or non-compliance with payer guidelines. Our service identifies the root causes of denials and implements corrective strategies to prevent recurrence, improving overall claim acceptance rates.
STATDOC's Revenue Cycle Management Solutions
Revenue Cycle Management
Optimize financial operations and billing processes for healthcare organizations, ensuring maximum reimbursement and reduced administrative burden.
RCM Data Analytics
Leverage advanced data analysis to uncover trends, identify revenue opportunities, and optimize billing and claims processes for superior financial performance.
Claims Management & Compliance
Ensure seamless claims submission, reduce denials, and maintain regulatory compliance to accelerate cash flow and protect revenue integrity.
RCM Strategy & Training
Develop robust RCM strategies and empower your staff with expert training in billing, coding, and financial performance optimization.

